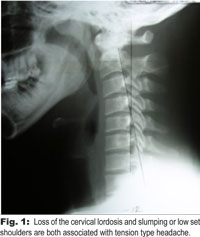
In my last two articles, I outlined why the unique degree of scientific validity and inter/intra examiner reliability of a postural approach to chiropractic are so important to the profession. Perhaps it’s time to take a look at the science behind why posture is so important to our patients as well. As it turns out, poor posture is of much more than just cosmetic concern.
In a word, postural imbalance hurts! Poor posture is associated with a wide range of clinical problems which present every day in your office. So, if you’ve been thinking postural subluxation is just some abstract concept, unrelated to you and your patients, let me assure you that that is not the case. Postural imbalance has very real clinical repercussions and there’s now a good body of research to back that up. For no particular reason, I’ve decided to discuss posture as it applies to tension headaches. And here, in no particular order of importance, are three studies worth reading about the relationship between postural imbalance and tension headache.
Three Studies on Tension Headache and Postural Imbalance
Study # 1: In 1993, at Japan’s Nagoya University School of Medicine, X-ray studies on 372 patients with tension type headache were compared to those of 225 normal (pain free) subjects. Researchers were looking for any relationship between tension type headache and three factors: 1) straightened (hypolordotic) cervical spine, 2) “low set” shoulders and, 3) cervical spine instability. The vast majority of patients with tension type headaches were found to also have straightened cervical spines and low set shoulders, as compared to the asymptomatic control group. (Cervical spine instability did not seem to be clearly associated with tension headache.) The authors concluded that “both a straightened cervical spine and low-set shoulders may play an important role in the pathogenesis of tension-type headache and its accessory symptoms.”1

Study # 2: -In 2006, researchers at the University Rey Juan Carlos, in Madrid, writing in the journal Headache2, associated forward head posture with chronic tension type headache (CCTH). This blinded and controlled study compared twenty patients with CCTH, to twenty patients without headaches. Patients were assessed manually for the presence of both active and latent trigger points and photographically in both standing and seated postures for the presence of forward head posture. The results were revealing.

In terms of posture, the headache patients showed significantly greater forward head position in both seated and standing positions than the control group. Even more interesting, 13 out of 20 headache patients demonstrated active trigger points in the subocciputal muscles and, incredibly, the remaining 7 CCTH patients demonstrated latent trigger points as well. (That’s 100 percent!) Not surprisingly, patients with more pronounced forward head posture and active trigger points experienced headaches of greater intensity and frequency than did patients with only latent trigger points. The author’s conclusions? Forward head posture “correlated positively with headache duration, headache frequency, and the presence of suboccipital active Trigger Points.”
It’s worth mentioning here that the authors don’t state that forward head posture is actually the direct cause of headache. The study merely points out a positive association between bad posture, active trigger points, and headache pain. Given that we routinely see asymptomatic patients with pronounced postural imbalance, it’s probably more reasonable that head forward postures are eventually causal in the development of myofascial trigger points and, subsequently, the onset of pain.
Study # 3– This 1993 paper3 observed a group of 47 patients aged 18-55 with both tension type (muscle contraction) headaches and common migraines. Subjects were examined using a standardized headache history, both static spinal radiographs, and pressure algometry among other methods. Seventy-seven percent of all subjects exhibited “a marked reduction, absence or reversal of the normal cervical lordosis.” Pressure algometry revealed that 85% of the muscle contraction headache patients “had at least one verifiable tender point in the upper cervical region.” The authors don’t state whether or not these tender points were actually true trigger points or not; but, in light of the previous Spanish study’s results, it seems likely they may have well been a mixture of both active and latent trigger points.
The authors concluded that both migraine and tension headache patients demonstrated high rates of neck pain during headache, tenderness in the occiputal areas, and cervical hypolordosis/kyphosis and that mechanical problems in the neck were playing an “important, but largely ignored role” in the generation of headache pain.
So here are three studies, documenting the interplay between postural imbalance and the common tension type headache. So, let me ask you Doctor, how many headache patients have you seen in your career? Answer…about a zillion. And how many of them had tender or trigger points in their neck musculature? Answer…nearly all of ’em. And, finally, how many of your current crop of headache patients have a reduction or loss of their cervical lordosis? Well, only you can really know the answer to that last question. But, I’m willing to bet your patients aren’t much different than the folks in these three studies.
Unfortunately, most doctors aren’t even bothering to measure the cervical lordosis and don’t understand the real secrets to truly correcting the lordotic curves. I’ll show you how to accurately differentiate and measure the various cervical configurations which walk into your office every day and how some of the best doctors in the country are getting the best corrections of their career.
Dr. Mark Payne is president of Matlin Mfg., a manufacturer and distributor of postural rehab products since 1988. For a FREE, unabridged copy of this article or other information on postural chiropractic, please contact Matlin Mfg. Inc. at 1-334 448 1210 or on the web at
www.MatlinMfg.com.
References:
1. Roentgenographic findings of the cervical spine in tension-type headache. Nagasawa A, Sakakibara T, Takahashi A. Headache. 1993 Feb;33(2):90-5.
2. Trigger points in the suboccipital muscles and forward head posture in tension-type headache. Fernández-de-las-Peñas C, Alonso-Blanco C, Cuadrado ML, Gerwin RD, Pareja JA. Headache. 2006, Mar;46(3):454-60.
3. Cervicogenic dysfunction in muscle contraction headache and migraine: a descriptive study. Vernon H, Steiman I, Hagino C. J Manipulative Physiol Ther. 1992 Sep;15(7):418-29.