:dropcap_open:M:dropcap_close:editation can be defined as a practice of concentrated focus upon a sound, object, visualization, breathing, or movement, or as attention in order to increase awareness of the present moment, reduce stress, promote relaxation, and enhance personal and spiritual growth. It is a self-directed activity that aims to keep the mind anchored in the present moment by focusing on a single object or breath pattern.

The practice of meditation is a self-directed process that shifts awareness to take focus away from the usual conditioning of our minds and thinking, which is often developed through our habits and usually without conscious intent. When the mind becomes quiet through meditation, a quiet stillness arises from the balance of body, mind, and spirit that, in turn, relaxes our nervous system. When we tap into our inner power by meditation, we can experience a transformation of the body, mind, and spirit.
Many consider meditation to be sitting alone quietly pondering, but true meditation is much more than relaxation. It is a state in which the mind is calm and at peace yet completely alert. Rather than “tuning out,” true meditation is a means of “tuning in.” This level of equanimity and centeredness is often referred to as being the “watchful witness of your thoughts.”
The practice of meditation dates back thousands of years in the Eastern religious practices of India, China, and Japan. Its resurgence in recent times began when Western medical researchers such as Herbert Benson, MD discovered the healing power of meditative practice. Meditation has been recommended for an array of physical ailments, including stress reduction, anxiety, insomnia, pain, depression, chronic illnesses such as heart disease, cancer, and HIV/AIDS, and overall wellness.
Types of Meditation
There are various types of meditation techniques throughout the world, including mindfulness, zazen, Zen meditation, transcendental meditation, kundalini, qigong, guided meditation or guided imagery techniques, heart rhythm meditation, various spiritual meditation or centering prayers, focused meditation, movement or walking meditation, and mantra meditation. The focus of this article is mindfulness meditation with breath as the anchor. It is also the subject of the “Guided Meditations” audio series (available on iTunes and at
www.guided-meditationssite.com).
Breath Awareness in Meditation
Breathing varies across meditation types with some meditation practices prescribing passive breathing and others using the breath as the sole point of focus when meditating. With this approach, you become aware of how each breath moves in your abdomen and how it feels as it moves in and out of your nostrils or mouth. The practice of breath awareness requires an open mind without trying to change the breathing pattern.
Breath awareness then becomes an anchor for mindfulness meditation. Meditation experts suggest abdominal breathing where the nostrils inhale the breath but the focus is on the belly rising and falling as you inhale and exhale. It is considered more efficient than normal chest breathing because it achieves a greater exchange of air.
Beginners can use paced breathing as a concentration meditation practice. A study by Park and Park (2012) found that paced breathing results in increased internal attention, which is a marker of successful meditation.
Meditation Postures
Having a good posture for meditation helps you focus on the meditation and ensures that the mind and body are connected. Whether you prefer to sit on a chair or on the floor, your spine should be erect and your body relaxed. Your hands should rest on your lap, palms down. You should be comfortable in the posture you choose for meditation. Sitting erect with the back, neck, and shoulders relaxed is a good posture.
The most commonly recommended meditation posture is the lotus position, which is traditionally considered to be the best posture for meditation. Sitting firmly on the floor, your body is erect and head well balanced in this posture. You can meditate longer in this position, but some people experience knee and joint pain with this posture.
Science Behind Meditation and Its Effects on the Body
As a doctor of chiropractic, the “above-down-inside-out” viewpoint of the benefits of meditation is often easy for us to understand. As science continues to substantiate the effectiveness of chiropractic manipulation for a variety of ailments, we should also be aware that there is a growing body of evidence for the practice of meditation. The interplay of perception and focus in the area of pain management suggests that meditative practice can be beneficial for a variety of physical ailments. For example, researchers at Stanford University’s Neuroscience and Pain Lab found that as patients watched their own brains react to pain in real-time, they could learn to control their responses. There was strikingly more activity in the brain when patients focused on something distracting instead of the pain.
Autonomic Nervous System and Meditation
The autonomic nervous system consists of the sympathetic and parasympathetic nervous systems. It is proposed that meditation can reduce the activity of the sympathetic nervous system while increasing activity in the parasympathetic nervous system. Most meditative activity targets the autonomic nervous system, which in turn regulates organs and muscles in the body and controls the digestive system, breathing, etc. Meditation may affect both sympathetic and parasympathetic nervous systems.
The “fight or flight” response is the body’s innate ability to “fight” or “flee” from perceived danger or harm to survival. When under stress due to internal or external situations, the body triggers the “fight or flight” response. This response is built into the brain to guard us from danger. The hypothalamus region of the brain is stimulated during stress and in turn it triggers a nerve cell action that stimulates the release of catecholamines (hormones) into the bloodstream to prepare us to run away or fight. When this occurs, the body undergoes changes causing a significant increase in breathing rate. The pupils dilate and arms and legs are pumped with blood to flee or fight, as required. The perception of pain reduces and we become more aware. Our bodies prepare us physically and physiologically for the situation. The “fight or flight” response creates tremendous movement and exertion and the stress hormones released are metabolized. Once the threat is over, body and mind return to a state of calm.
Meditation helps the body release catecholamines and other stress hormones as parasympathetic activity increases in the body. In response to stress, the hypothalamus in the brain is activated and triggers the adrenal gland to produce and release the stress hormone cortisol.
Catecholamines are certain chemical messengers that include dopamine, norepinephrine, and epinephrine. The response also affects the heart, lungs, and blood circulation in the body. In a study (Jung YH et al. 2010), catecholamines were measured in meditation and control groups, and it was found that the levels are related to stress levels. The meditation group showed higher scores on positive effect and lower scores on stress compared with the control group.
Health Benefits of Meditation
For years researchers have studied the effects of meditation and reported that it calms stress, depression, and anxiety. However, what else might we be gaining from meditation? Data analysis from multiple studies has shown that the effect of meditation is not only a mental process, but surprisingly, a physiological process as well. Meditation has the potential to aid in treating heart disease, depression, and insomnia. Research also suggests that regular meditative practices can reduce pain and enhance the body’s immune system.
:dropcap_open:The interplay of perception and focus in the area of pain management suggests that meditative practice can be beneficial for a variety of physical ailments.:quoteleft_close:
A 1995 report to the National Institutes of Health on alternative medicine concluded that “more than 30 years of research, as well as the experience of a large and growing number of individuals and health care providers, suggests that meditation and similar forms of relaxation can lead to better health, higher quality of life, and lowered health care costs…” Mind-body therapy is the most common form of complementary and alternative medicine used in the United States. Meditation, relaxation, breathing techniques, yoga, etc. are used to treat pain, stroke, headaches, fibromyalgia, epilepsy, and many other neurological diseases. Mind-body therapies focus on the interactions between the brain, mind, body, and our behavior, and how those interactions affect our health and diseases.
Most of these therapies are linked to relaxation and, therefore, are beneficial to patients suffering from psychological stress. Mind-body therapies like meditation are easy to utilize due to low associated risk and low cost. The self-directed nature of meditations allows patients to actively manage their treatments. Different meditation types include self-observation of mental activity and mindfulness, which means focusing on internally generated events such as breathing, emotions, and thoughts.
Application of Meditation to Neurologic Processes
The most common neurological conditions that mind-body therapies are applied to are pain syndromes. Patients suffering from chronic pain have been treated successfully with meditation. Meditation and other forms of mind-body therapies are used frequently among adults suffering from common neurological conditions such as headaches and general pain.
Headaches
Mindful meditation helps control severe headaches and discomfort, and is a cost-effective alternative to pain medications. As chiropractors know, headaches are not attributed to a single pathogenesis, and often involve various dysfunctional mechanisms such as joint dysfunction, myofascial restriction, vascular changes, neurological dysafferentation, and postural sequelae. Meditation alone or in combination with other mind-body therapies has been shown to significantly reduce symptoms of migraine, tension, and mixed-type headaches.
Wachholtz and Pargament (2008) studied patients suffering from migraine headaches and investigated if spiritual medicine was effective in enhancing pain tolerance to reduce migraine-related symptoms. They found that people who practiced spiritual meditation had a greater decrease in migraine headache frequency as well as anxiety. The subjects also showed a greater increase in pain tolerance.
Back and Neck Pain
Different chronic pain conditions are often relieved with mind-body therapies. Back and neck pain are the most common chronic pain syndromes seen in chiropractic offices, and several studies have focused on the benefits of mind-body therapies to manage spinal pain symptoms.
An 8-week mindfulness-based stress reduction program showed significant change in pain intensity among patients suffering from arthritis and back and neck pain (Rosenzweig et al. 2010). A 10-week mindfulness meditation program targeted to train chronic pain patients in self-regulation with pain in the lower back, neck and shoulder, and headache. At the end of 10 weeks, 65% of the patients showed reduction greater than or equal to 50% (Kabat-Zinn J. 1982).
Older patients with chronic lower back pain benefitted tremendously from a mindfulness meditation program such as the one featured at
www.guided-meditationssite.com. Based on their diary entries, participants described improved attention skills and quality of sleep. Common themes were identified that related to pain reduction, improved attention, and overall well-being, suggesting that mindfulness meditation has potential as a nonpharmacologic agent in the treatment of chronic pain for older adults (Morone et al. 2008). Many study participants noted pain reduction and indicated the methods and processes that were used to reduce the pain, i.e., distraction from pain, pain reduction using meditation, heightened awareness of pain that led them to make behavioral changes, and to develop better coping mechanism to pain. Some of the mechanisms the older adults used to distract themselves are simple and we can all do this to cope with pain. Some focused on other parts of the body while others focused on routine activities.
One of the mechanisms the older adults used was to develop a heightened awareness of body sensations that led to behavior change eventually resulting in reducing pain. They were able to recognize pain earlier than was typical by awakened realization of the body’s subtle sensations. This allowed them to intervene before the pain became severe. When the adults are able to cope better, diary entries such as this were common: “The pain is still with me; however, it just doesn’t feel as intense as it was.” Distraction from pain with music, relaxation, prayer, and exercise helped the participants with pain relief. Mindfulness meditation was shown to be effective in relieving pain when the focus is on breathing or concentration was somewhere other than the pain.
The equanimity that meditation affords the practitioner with freedom from pain is described by Kabat-Zinn (1982) as “an attitude of detached observation toward a sensation when it becomes prominent in the field of awareness, and to observe with similar detachment the accompanying but independent cognitive processes, which lead to evaluation and labeling of the sensation as painful, as hurt.” It is this focus on relaxation and breath work that I used when designing the audio meditation that I’ve recently made available for download. By sharing this system with your patients, you can make a positive impact on their overall health.
Our body naturally wishes to avoid pain and that is translated as anxiety. To be present with pain when it arises is difficult, but with mindfulness we can learn to come to peace with pain. Pain can be debilitating and anxiety resides with the pain to magnify suffering. Learning to differentiate the pain and how the body reacts to the pain is useful in that our reactions do not need to be added to the physical pain.
Final Thoughts
Meditation has a long history with a recent resurgence in the healthcare arena. Its philosophies (above-down-inside-out, focus on balance and homeostasis), physical practice (proper posture, diaphragmatic breathing), and growing body of scientific studies (consistent with the evidence-based care paradigm) make it an excellent adjunct to chiropractic patient care. Both disciplines share an art-philosophy-science paradigm that can produce positive changes in the body-mind.
Dr. Douglas J. Taber has been referred to as the scholar-sage of integrated chiropractic care. He is the author of multiple books and articles, and his 2011 release, The Neck Pain Solution: A Guided Healing Approach, was winner of the 2011 International Book Awards. This article is an excerpt from his upcoming book, Here, scheduled for release in late 2013. His recent audio release, Guided Meditations, is available on iTunes and Amazon. For more information, go to www.guided-meditationssite.com. He can be reached for speaking engagements and book signings at [email protected].
References:
Kox M et al. The influence of concentration/meditation on autonomic nervous system activity and the innate immune response: a case study. Psychosom Med. 2012 Jun;74(5):489-94.
Peressutti C et al. Does mindfulness meditation shift the cardiac autonomic nervous system to a highly orderly operational state? Int J Cardiol. 2012 Jan 26;154(2):210-2.
Peng CK et al. Exaggerated heart rate oscillations during two meditation techniques. Int J Cardiol. 1999 Jul 31;70(2):101-7.
Jung YH et al. The effects of mind-body training on stress reduction, positive affect, and plasma catecholamines. Neurosci Lett. 2010 Jul 26;479(2):138-42.
Jung YH et al. Influence of brain-derived neurotrophic factor and catechol O-methyl transferase polymorphisms on effects of meditation on plasma catecholamines and stress. Stress. 2012 Jan;15(1):97-104.
Lang R et al. Sympathetic activity and transcendental meditation. J Neural Transm. 1979;44(1-2):117-35.
Michaels RR, Huber MJ, McCann DS. Evaluation of transcendental meditation as a method of reducing stress. Science. 1976 Jun 18;192(4245):1242-4.
Infante JR et al. Catecholamine levels in practitioners of the transcendental meditation technique. Physiology & Behavior. 2001; 72:141-6.
Wahbeh H et al. Mind-body interventions. Neurology. 2008;70:2321-28.
Astin JA. Mind-body therapies for the management of pain. Clin J Pain. 2004 Jan-Feb;20(1):27-32.
Sun TF, Kuo CC, Chiu NM. Mindfulness meditation in the control of severe headache. Chang Gung Med J. 2002 Aug;25(8):538-41.
Sierpina V, Astin J, Giordano J. Mind-body therapies for headache. Am Fam Physician. 2007 Nov 15;76(10):1518-22.
Rosenzweig S et al. Mindfulness-based stress reduction for chronic pain conditions: variation in treatment outcomes and role of home meditation practice. J Psychosom Res. 2010 Jan;68(1):29-36.
Wachholtz AB, Pargament KI. Migraines and meditation: does spirituality matter? J Behav Med. 2008 Aug;31(4):351-66.
Kabat-Zinn J. An outpatient program in behavioral medicine for chronic pain patients based on the practice of mindfulness meditation: theoretical considerations and preliminary results. Gen Hosp Psychiatry. 1982 Apr;4(1):33-47.
Morone NE, Lynch CS, Greco CM, Tindle HA, Weiner DK. “I felt like a new person.” The effects of mindfulness meditation on older adults with chronic pain: qualitative narrative analysis of diary entries. J Pain. 2008 Sep;9(9):841-8.
Kabat-Zinn J, Lipworth L, Burney R. The clinical use of mindfulness meditation for the self-regulation of chronic pain. J Behav Med. 1985 Jun;8(2):163-90.
Kabat-Zinn J. An outpatient program in behavioral medicine for chronic pain patients based on the practice of mindfulness meditation: theoretical considerations and preliminary results. Gen Hosp Psychiatry. 1982 Apr;4(1):33-47.
Morone NE, Greco CM. Mind-body interventions for chronic pain in older adults: a structured review. Pain Med. 2007 May-Jun;8(4):359-75.
Bonadonna R. Meditation’s impact on chronic illness. Holist Nurs Pract. 2003 Nov-Dec;17(6):309-19.
Balaji PA, Varne SR, Ali SS. Physiological effects of yogic practices and transcendental meditation in health and disease. N Am J Med Sci. 2012 Oct;4(10):442-8.
Park YJ, Park YB. Clinical utility of paced breathing as a concentration meditation practice. Complement Ther Med. 2012 Dec;20(6):393-9.
Kiran et al. Impact of meditation on autonomic nervous system—a research study. 2011Sept-Dec;1(1):144-8.
Takahashi T et al. Changes in EEG and autonomic nervous activity during meditation and their association with personality traits. Int J Psychophysiol. 2005 Feb;55(2):199-207.
Rosenkranz MA et al. A comparison of mindfulness-based stress reduction and an active control in modulation of neurogenic inflammation. Brain, Behavior, and Immunity. 2013 Jan (27):174–84.
 In school, I was taught that chiropractic was a philosophy, an art, and a science. That paradigm bothered me for 35 years, so I decided to create my own; a new paradigm for the 21st century, and one that remains at the center of all my teaching: “Chiropractic is a science that has an art and embraces a philosophy.”
In school, I was taught that chiropractic was a philosophy, an art, and a science. That paradigm bothered me for 35 years, so I decided to create my own; a new paradigm for the 21st century, and one that remains at the center of all my teaching: “Chiropractic is a science that has an art and embraces a philosophy.”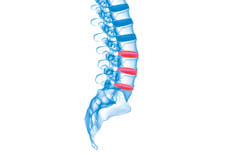
 Following recent publication of a rat study that indicated differences in gut microbial concentrations at the time of type 1 diabetes onset, the authors designed a small human study to test their hypothesis that type 1 diabetes in humans could also be linked to specific microbes in the human gut.
Following recent publication of a rat study that indicated differences in gut microbial concentrations at the time of type 1 diabetes onset, the authors designed a small human study to test their hypothesis that type 1 diabetes in humans could also be linked to specific microbes in the human gut.
 This paper, a 2012 study from Spine, examined the relationship between posture and spinal pain in young people. The authors looked at 1,196 Flemish adolescents. The average age of the 639 male participants was 12.6 years; it was 10.6 years for the 557 females. The authors acknowledge that data relating posture to pain, particularly in young people, are “sparse.” As a profession, chiropractors historically have placed a great deal of emphasis on the relationship between spinal structure and spinal pain, although that emphasis has waned in recent decades. In spite of our profession’s history, a number of previous studies, several of which looked at the status of the spinal curves, have failed to show any clear correlation between posture and spinal pain. Other studies that focused more on regional or segmental misalignment have also failed to show a correlation between spinal structure and pain.
This paper, a 2012 study from Spine, examined the relationship between posture and spinal pain in young people. The authors looked at 1,196 Flemish adolescents. The average age of the 639 male participants was 12.6 years; it was 10.6 years for the 557 females. The authors acknowledge that data relating posture to pain, particularly in young people, are “sparse.” As a profession, chiropractors historically have placed a great deal of emphasis on the relationship between spinal structure and spinal pain, although that emphasis has waned in recent decades. In spite of our profession’s history, a number of previous studies, several of which looked at the status of the spinal curves, have failed to show any clear correlation between posture and spinal pain. Other studies that focused more on regional or segmental misalignment have also failed to show a correlation between spinal structure and pain. 
 At the six-week interval, the patient received a letter from AllFarm Insurance Company stating that an IME has been ordered to determine the necessity of care. The patient showed up at the appointed time for the examination with a friend who joined him during the examination and handed the IME doctor a copy of the MRI on a disc and submitted for examination. The IME doctor spent a total of four or five minutes with the patient, which included the time he spent obtaining the history and doing a physical exam. He released the patient from the examination by walking out in front of the patient and never seeing him ambulate. Two weeks later, the patient and treating doctor received letters from the carrier stating that all future benefits were denied and three out of the six previous weeks’ benefits were denied as well. Upon request of the IME doctor’s report, the treating doctor and patient found the IME doctor stated the diagnosis as lumbar spine strain/sprain resolved.
At the six-week interval, the patient received a letter from AllFarm Insurance Company stating that an IME has been ordered to determine the necessity of care. The patient showed up at the appointed time for the examination with a friend who joined him during the examination and handed the IME doctor a copy of the MRI on a disc and submitted for examination. The IME doctor spent a total of four or five minutes with the patient, which included the time he spent obtaining the history and doing a physical exam. He released the patient from the examination by walking out in front of the patient and never seeing him ambulate. Two weeks later, the patient and treating doctor received letters from the carrier stating that all future benefits were denied and three out of the six previous weeks’ benefits were denied as well. Upon request of the IME doctor’s report, the treating doctor and patient found the IME doctor stated the diagnosis as lumbar spine strain/sprain resolved.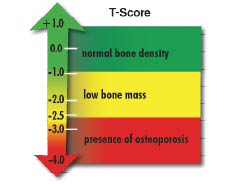
 Increased thoracic kyphosis is associated with osteoporosis and results in a reduced quality of life (QOL). It is also associated with alteration of postural balance, resulting in increased risk of falling. Falls in the geriatric population are associated with increased incidence of fracture.2 Among older adults (those 65 or older), falls are one of the leading causes of injury and death. They are also the most common cause of nonfatal injuries and hospital admissions for trauma. In 2010, 2.3 million nonfatal fall injuries among older adults were treated in emergency departments and more than 662,000 of these patients were hospitalized.3
Increased thoracic kyphosis is associated with osteoporosis and results in a reduced quality of life (QOL). It is also associated with alteration of postural balance, resulting in increased risk of falling. Falls in the geriatric population are associated with increased incidence of fracture.2 Among older adults (those 65 or older), falls are one of the leading causes of injury and death. They are also the most common cause of nonfatal injuries and hospital admissions for trauma. In 2010, 2.3 million nonfatal fall injuries among older adults were treated in emergency departments and more than 662,000 of these patients were hospitalized.3 
 As a full-service Third Party Administration firm (TPA), we welcomed the “full disclosure” of fees promulgated by recent Labor Department regulations. Naïvely, we believed this would open the eyes of plan sponsors to the exorbitant fees charged by the typical mutual-fund sponsored plans, payroll company plans, or any of the other “bundled” plans offered by many in the financial advisory community. Sadly, the disclosures were done in such a way that few took notice.
As a full-service Third Party Administration firm (TPA), we welcomed the “full disclosure” of fees promulgated by recent Labor Department regulations. Naïvely, we believed this would open the eyes of plan sponsors to the exorbitant fees charged by the typical mutual-fund sponsored plans, payroll company plans, or any of the other “bundled” plans offered by many in the financial advisory community. Sadly, the disclosures were done in such a way that few took notice.
 :dropcap_open:I:dropcap_close: talk to a lot of chiropractors across the country. My business, Matlin Manufacturing Inc., brings me into contact with doctors with a wide range of backgrounds and techniques. The number of techniques and therapeutic modalities used by chiropractors is extremely varied. Almost without exception, the vast majority of chiropractors I’ve spoken with still center much of their treatments for spinal pain around the use of spinal manipulation. Manual manipulation of the spine is most often rendered in the form of high-velocity/low-amplitude (HVLA) adjustments. So in spite of all the observed differences between chiropractors of varying backgrounds, this one commonality seems to remain for the majority of doctors.
:dropcap_open:I:dropcap_close: talk to a lot of chiropractors across the country. My business, Matlin Manufacturing Inc., brings me into contact with doctors with a wide range of backgrounds and techniques. The number of techniques and therapeutic modalities used by chiropractors is extremely varied. Almost without exception, the vast majority of chiropractors I’ve spoken with still center much of their treatments for spinal pain around the use of spinal manipulation. Manual manipulation of the spine is most often rendered in the form of high-velocity/low-amplitude (HVLA) adjustments. So in spite of all the observed differences between chiropractors of varying backgrounds, this one commonality seems to remain for the majority of doctors. 
 In addition to the possible mistakes that can be made on the CMS-1500 claim form, you have to consider what potential problems can arise after you have verified a patient’s insurance coverage and benefits. Even after all the correct steps have been followed carefully in the verification process and you have received a verbal and written explanation of benefits, claims can still be denied for payment due to an error on the carrier’s part. When you are accepting an insurance assignment and mistakes happen (e.g., errors in copays or deductible amounts, etc.), if it is discovered that patients actually owe more than what they were told they owed and have already paid (as the result of misquoting benefits), chances of collecting are often slim. Moreover, it can leave patients with a negative reminder of your financial policies. It sometimes becomes a vicious cycle. It can take weeks to discover if the carrier misquoted benefits and as a result, insufficient (wrong) amounts were collected from the patient. This is one reason why the carrier continually reminds us during every step of the verification cycle that “benefit details are not a guarantee of payment!”
In addition to the possible mistakes that can be made on the CMS-1500 claim form, you have to consider what potential problems can arise after you have verified a patient’s insurance coverage and benefits. Even after all the correct steps have been followed carefully in the verification process and you have received a verbal and written explanation of benefits, claims can still be denied for payment due to an error on the carrier’s part. When you are accepting an insurance assignment and mistakes happen (e.g., errors in copays or deductible amounts, etc.), if it is discovered that patients actually owe more than what they were told they owed and have already paid (as the result of misquoting benefits), chances of collecting are often slim. Moreover, it can leave patients with a negative reminder of your financial policies. It sometimes becomes a vicious cycle. It can take weeks to discover if the carrier misquoted benefits and as a result, insufficient (wrong) amounts were collected from the patient. This is one reason why the carrier continually reminds us during every step of the verification cycle that “benefit details are not a guarantee of payment!”
 The practice of meditation is a self-directed process that shifts awareness to take focus away from the usual conditioning of our minds and thinking, which is often developed through our habits and usually without conscious intent. When the mind becomes quiet through meditation, a quiet stillness arises from the balance of body, mind, and spirit that, in turn, relaxes our nervous system. When we tap into our inner power by meditation, we can experience a transformation of the body, mind, and spirit.
The practice of meditation is a self-directed process that shifts awareness to take focus away from the usual conditioning of our minds and thinking, which is often developed through our habits and usually without conscious intent. When the mind becomes quiet through meditation, a quiet stillness arises from the balance of body, mind, and spirit that, in turn, relaxes our nervous system. When we tap into our inner power by meditation, we can experience a transformation of the body, mind, and spirit.
 Elastic therapeutic taping has taken off in the United States as an exciting addition to the manual therapist’s treatment toolbox. Since the 2008 Olympics, a slew of elastic tapes have made their way onto the market, touting their therapeutic benefits. As a Certified Kinesio Taping® Instructor (CKTI), I have learned that each brand of elastic therapeutic tape shares some of the properties of Kinesio Tape, but no other tape shares all of its properties. As the properties of each tape are unique—variations include thread count in the material, the degree of elasticity, the amount of recoil and the amount and quality of adhesive—one cannot generalize application methods across brands of elastic therapeutic tape. Each brand must be used in a way that is appropriate for the target population and with application methods designed for its particular properties. My goal here is to educate the reader specifically about the KTM and demystify its particular therapeutic effects.
Elastic therapeutic taping has taken off in the United States as an exciting addition to the manual therapist’s treatment toolbox. Since the 2008 Olympics, a slew of elastic tapes have made their way onto the market, touting their therapeutic benefits. As a Certified Kinesio Taping® Instructor (CKTI), I have learned that each brand of elastic therapeutic tape shares some of the properties of Kinesio Tape, but no other tape shares all of its properties. As the properties of each tape are unique—variations include thread count in the material, the degree of elasticity, the amount of recoil and the amount and quality of adhesive—one cannot generalize application methods across brands of elastic therapeutic tape. Each brand must be used in a way that is appropriate for the target population and with application methods designed for its particular properties. My goal here is to educate the reader specifically about the KTM and demystify its particular therapeutic effects.