The topic of spondylolysis and/or spondylolisthesis has been clouded with confusion for many years. To understand the true etiology as a stress fracture rather than an inherited congenital anomaly or predisposition has been a lifelong quest for me. The normally developing pars interarticulares is a fully ossified structure at birth and without a local synchondrosis to undergo nonunion. There has never been a patient born with a lumbar spondylolysis and/or spondylolisthesis. The true etiology of spondylolysis (pars defects) is that of a stress fracture, which is, in fact, a fatigue fracture where repetitive stress on normal bone allows the bone to fatigue, much like you see in the metatarsal bones and tibia with marathon runners and gymnasts.
To fully understand the concept of the pain-generating factors associated with spondylolysis and/or spondylolisthesis, one must look beyond plain films and computed tomography to more physiological imaging. In the past, I have stressed the importance of determining the presence/absence of increased physiological activity at the pars interarticularis as an aid to developing an accurate diagnosis and appropriate treatment plan for patients who have or are at risk for spondylolysis, coining the term “PENDING SPONDYLOLYSIS” for those who have a developing stress fracture without frank separation. Historically, two modes of diagnostic imaging have been used to assess whether physiologic activity is present and associated with existing pars defects. Radionuclide bone scan imaging, particularly SPECT (Single Photon Emission Computed Tomography), has often been the examination of choice, however suffers from two drawbacks; it does expose the patient to ionizing radiation and it provides very little anatomical information. Fortunately, these concerns have been addressed with the advent of MR imaging.

Having reviewed thousands of cases, often with sports related back pain and/or spondylolysis, I have had the opportunity to see proven value of MR imaging for evaluation of the physiological activity that occurs adjacent to a pars defect, or that which is hidden in the region of the pars interarticularis when the defect is, in fact, “PENDING”. I feel, at this point in time, that SPECT imaging is probably no longer the exam of choice, since there is so much more information obtained with the physiological imaging of magnetic resonance. Additionally, the exquisite anatomical information that MR imaging provides can be invaluable in demonstrating other possible causes of back pain in those individuals whose MR findings are negative for spondylolysis. The ability to evaluate the spinal canal, exiting nerve roots and the integrity of the discs, along with the surrounding paraspinal musculature, offers so much more information in the evaluation of a young athlete with persistent back pain with what is often repetitive hyperextension.
Let’s STIR Things Up in the Evaluation of Spondylolysis and/or Spondylolisthesis
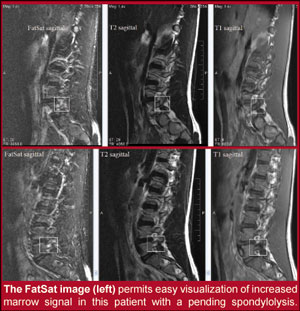
I have seen many cases where bone marrow edema adjacent to the pars or hidden within an intact pars on its way to becoming a pars defect (PENDING SPONDYLOLYSIS) has been missed on standard T2-weighted images, where a STIR imaging sequence clearly provides this information. At this point in time, I offer to the profession that an MRI scan should be the exam of choice, with the proviso that the MR protocol includes a strongly fluid sensitive pulse sequence, such as STIR (short-tau inversion recovery) or other strong fat-suppression protocol. When appropriate clinical management depends on whether the spondylolysis and/or spondylolisthesis is active and/or inactive, only physiological activity will provide that information. If your local imaging center does not include STIR or other fat-suppressed (FatSat) pulse sequence as part of their routine lumbar MRI scan, requesting a sagittal STIR imaging will definitively answer the question of normal or increased physiological activity in the region of the pars interarticularis. When ordering this additional study to the standard lumbar spine MRI scan, it will only add a few minutes to the overall imaging time and should add no additional expense to the study.

Spondylolysis should be included in the differential for any patient who complains of low back pain due to repetitive hyperextension, be it sports or industrial related. Physical exam findings such as a positive Stork (single leg hyperextension) test, often positive in acute facet syndrome and/or hot pars abnormality, may further indicate the need for more physiological imaging of the region of the lower lumbar pars interarticularis. When repeating an MRI scan to evaluate whether the bone marrow edema adjacent to the pars has subsided and the patient can be removed from the standard Boston overlap brace that the patient has been placed in, the only imaging sequence really required to determine that the active pars defect has become inactive is the sagittal STIR fluid-sensitive imaging sequence. This should be performed after the patient has been in a Boston overlap brace for a minimum of three to four months and, if the imaging study shows no evidence of persistent edema, one can allow the patient to slowly go back to their sports or work related physical activities. Core stabilization exercises and physical activity back to their normal routines should occur slowly, and some common sense should be used by the clinician in not allowing the athlete to go back at full performance too quickly. For a more detailed discussion of this condition, see Chapter 5 of the new edition of Essentials of Skeletal Radiology, published in 2005 by Lippincott Williams & Wilkins. Included there are some positive treatment protocols for patients with active spondylolysis and/or spondylolisthesis.
As a final comment, it is always appropriate and very useful to the radiologist for the referring clinician to clearly state on the imaging request form the working diagnosis. Tell the radiologist why imaging is being performed and what questions you are trying to answer. This is particularly important in the evaluation of spondylolysis, so that right imaging sequences are performed and the sometimes subtle changes in marrow signal are not overlooked. Including a copy of the material in Chapter 5 of my textbook covering “Active versus Inactive Spondylolisthesis” and perhaps a copy of the article which I have referenced in this text along with your imaging request may also be useful for emphasis. The additional information may help the medical radiologist to provide you the right report and ensure proper and complete evaluation of the patient’s presenting complaint.
Thanks to Dr. Jeff Thompson, Professor and Chairman, Department of Radiology, Texas Chiropractic College, Houston, Texas, for his help in preparation of the text and images for this article.
Dr. Terry R. Yochum is a second generation chiropractor and a Cum Laude Graduate of National College of Chiropractic, where he subsequently completed his radiology residency. He is currently Director of the Rocky Mountain Chiropractic Radiological Center in Denver, Colorado, and Adjunct Professor of Radiology at the Southern California University of Health Sciences, as well as an instructor of skeletal radiology at the University of Colorado Schoolof Medicine, Denver, CO. Dr. Yochum can be reached at 1-303-940-9400 or by e-mail at [email protected].
References
1. Yochum, TR, Rowe, LJ: Essentials of Skeletal Radiology, 3rd ed., Chapter 5,Williams & Wilkins, Baltimore, Maryland, 2005
2. Yochum, T.R., et al., Active or Inactive Spondylolysis and/or Spondylolisthesis: What’s the Real Cause of Back Pain? J.N.M.S: Journal of the Neuromusculoskeletal System, Vol. 10, No. 2, Summer 2002.