 :dropcap_open:I:dropcap_close:got a call from someone who sounded terrible.
:dropcap_open:I:dropcap_close:got a call from someone who sounded terrible.
“Doctor Koren, I’m in agony. A few days ago I was out golfing with my family and something went out in my back. I’ve been in bed for days. Yesterday, I was literally carried to get an MRI and a neurosurgeon will be getting back to me soon. A friend who saw you said you can help me. Can you do anything for me?”
“Can you come over to my office?”
“I can’t get out of bed. I haven’t shaved in days. I can’t move. Can you come here?”
“Of course.”
I got his address, picked up my arthrostim adjusting instrument and was off.
When I arrived at his house, his wife let me in. “Please follow me, he’s upstairs in bed; he’s been counting the seconds until you arrived.”
I followed her upstairs.
It looked like he had not left his bed for many days. He had a 5 or 6-day-old beard.
“Thank you so much for coming. Please excuse me for not getting up.”
“No problem, where’s an electrical outlet?” I plugged in the instrument and, quite literally, in the most professional way possible, climbed into bed with him.
“I haven’t showered in a few days,” he said.
“That’s OK,”I told him. “Neither have I.”
My getting into the bed moved the mattress and he grunted in pain. “I’ll try to move around slowly,” I told him.
I checked and adjusted him as he lay there. I adjusted what I could and it was no surprise that his discs as well as his vertebrae were subluxated. In addition, he was very dehydrated; disc problems and dehydration go together. He was playing golf on a very hot day and drinking margaritas. That’ll dry you out and it may have precipitated his disc damage.
Actually I’ve found that, if you get people with disc problems to drink more water, a large number of them would, by that act alone, become pain free. When discs are dehydrated, they become friable—the fibers crack and split. That can occur especially when they are under stress (such as swinging a golf club.)
I adjusted the discs and vertebra. He was still in a lot of pain. “I’ll see you tomorrow, I told him.”
The next day, as I entered the bedroom, he sat up in bed. He was able to move a little without too much pain and had even showered and shaved. He couldn’t stand very long and was still fairly immobile most of the time. I climbed into bed and worked on him again; this time I was able to reach more areas.
The next day, he was driven to my office and, using crutches, walked into the adjusting room. Because I was able to adjust him standing as well as sitting and in the position he was in as he swung his golf club, more subluxations were revealed and could be corrected.
The following day, he drove in by himself. After a few more days, he was pain free.
Later in the week, he drove himself to the neurosurgeon. As he walked into the doctor’s office, the MD’s jaw dropped. “Your MRI was the second worst train wreck I had ever seen in my 30 year career. I was going to recommend immediate surgery. I can’t believe you’re pain free. Amazing.”
“Would you like to know what I did to get out of pain?” he asked.
“No, not really.”
Surprised? I’m sure that if you’re a doctor of chiropractic reading this story you’ve got plenty of similar stories.
The number one rule in all healing is, “Listen to the patient; the patient is your teacher.” Of course, that only works if one’s mind is open.
Another example
This medical phenomenon is not only related to chiropractic care. For example, Harris Coulter, Ph.D., the world famous medical historian, cites a friend of his who was diagnosed with lung cancer and given six months to live. Dr. Coulter recalled, “I told him that, in Alexandr Solzhenitsn’s book, The Gulag Archipeligo, Solzhenitsn mentioned that he had been diagnosed with lung cancer and cured it after taking extracts from a yew tree.”
So, his friend found a source of yew extract and began to take it under the direction of a naturopathic physician. Six months later, he returned to the MD who had given him six months to live. After the examination, the doctor reported, “Your lungs are clear. No cancer at all.”
“Would you like to know what I did?”
“No, not really.”
Medical mis-education
I’m shocked that the medical profession ever questioned the intelligence, ethics and morality of chiropractors and other alternative healthcare practitioners. Apparently, they were looking in a mirror, blinded by the prestige, money and power that society has given them.
What is it with the medical mind? How can they be so clueless? Coulter discusses this in his magnum opus Divided Legacy, Vol. 4 in chapter 26, “The Training of Physicians,” (P. 645), where he quotes MD’s, educators and students. Coulter writes: “The majority of students complain that they experience constant anxiety and stress. A “dehumanizing experience” is their most frequent characterization of medical school….
:dropcap_open:From a sophomore: “I was not sure the day after I entered whether I was in a prison or a kindergarten, and I still haven’t made up my mind.” Daniel H. Funkenstein
The doctor-scientist orientation produces a nasty side effect; it takes incoming medical students who are interested in people and transforms them into doctors interested in diseases. Michael Crichton
Students entering medical school are a very healthy bunch of young people. If they’re not when they leave, it’s because we did it to them. Pearl Rosenberg:quoteleft_close:
Coulter continues: “The clinical years of medical school thus perpetuate the confusion and alienation of the preclinical ones. The first two years instill in the student just enough abstract information to inhibit precise observation, while the last two deaden the sensibilities which might have enabled him to overcome the legacy of the preclinical period. He leaves medical school dehumanized.”
Worshiping an idol?
These are people who are worshipped by the general public who are unaware of what kind of people they are putting their trust in. These are people who are caught in a machine that is as much political as it is professional. Their education is increasingly overseen by pharmacological research and they graduate with a narrow view of life and health. Perhaps they have no concept of health, since their focus is disease.
Is it any wonder that, when true healing is revealed, they recoil in shock and bewilderment? Fearful of admitting their deficiencies, they quickly turn away and mumble, “No, not really.”
And they are right. They don’t want real. Real is a frightening place. It is beyond the confines of their comfortable thoughts. There is no reality in their education, outlook and practice. They’re better off not going there; it would destroy their powerful, though brittle, world.
A bed call
That house call, or bed call, that I made was a microcosm of what many patients must deal with. This patient was lucky to have looked outside the system. Not everyone is lucky enough to have a chiropractor make a house call or open enough to invite one.
Tedd Koren, D.C., is the developer of Koren Specific Technique. For information, go to www.korenspecifictechnique.com. Dr. Koren also writes patient education materials. Go to www.korenpublications.com. Dr. Koren can be reached at [email protected].
 Exam Findings
Exam Findings 

 :dropcap_open:V:dropcap_close:
:dropcap_open:V:dropcap_close: Vitamin D deficiency is a serious medical condition that has been associated with an increased risk of developing cardiovascular disease, type 2 diabetes, hypertension, various cancers and autoimmune diseases. Vitamin D insufficiency occurs at epidemic levels in many industrialized countries, where exposure to sunlight tends to be limited and diets tend not to include sufficient amounts of foods naturally rich in vitamin D. During 2009, Dr. Guillory tested more than 1,200 of his patients and found that roughly 90 percent had sub-optimal vitamin D levels, as determined by serum 25(OH) vitamin D levels below 32 ng/mL. Dr. Guillory achieved great success in treating this with Bio-D- Mulsion Forte®, a microemulsified preparation made by Biotics Research Corporation.
Vitamin D deficiency is a serious medical condition that has been associated with an increased risk of developing cardiovascular disease, type 2 diabetes, hypertension, various cancers and autoimmune diseases. Vitamin D insufficiency occurs at epidemic levels in many industrialized countries, where exposure to sunlight tends to be limited and diets tend not to include sufficient amounts of foods naturally rich in vitamin D. During 2009, Dr. Guillory tested more than 1,200 of his patients and found that roughly 90 percent had sub-optimal vitamin D levels, as determined by serum 25(OH) vitamin D levels below 32 ng/mL. Dr. Guillory achieved great success in treating this with Bio-D- Mulsion Forte®, a microemulsified preparation made by Biotics Research Corporation. 20 full-time firefighters of the Aurora Fire Department were selected on a volunteer basis to participate in an eight-week study during the winter/spring months of 2009. Upon initiation of the study, the 20 subjects were advised to stop consuming multivitamins, cod liver oil and other supplements containing vitamin D. The subjects filled out a medical symptom questionnaire aimed to assess subjective indications of mood, energy level and digestive complaints. All subjects had blood drawn (at the Care Group, PC, office of Gerard Guillory MD in Aurora, Colorado ) and serum levels of 25- hydroxyvitamin D (25(OH)) vitamin D tested through Laboratory Corporation of America (Lab. Corp) via an assay developed by DiaSorin. The subjects were advised to take 4,000 IU/day (2 drops) daily of the liquid emulsified preparation produced by Biotics Research Corporation. After eight weeks of daily supplementation the study subjects 25(OH) vitamin D levels were retested by Laboratory Corporation of America. The subjects also filled out the same medical symptom questionnaire and the data was compiled.
20 full-time firefighters of the Aurora Fire Department were selected on a volunteer basis to participate in an eight-week study during the winter/spring months of 2009. Upon initiation of the study, the 20 subjects were advised to stop consuming multivitamins, cod liver oil and other supplements containing vitamin D. The subjects filled out a medical symptom questionnaire aimed to assess subjective indications of mood, energy level and digestive complaints. All subjects had blood drawn (at the Care Group, PC, office of Gerard Guillory MD in Aurora, Colorado ) and serum levels of 25- hydroxyvitamin D (25(OH)) vitamin D tested through Laboratory Corporation of America (Lab. Corp) via an assay developed by DiaSorin. The subjects were advised to take 4,000 IU/day (2 drops) daily of the liquid emulsified preparation produced by Biotics Research Corporation. After eight weeks of daily supplementation the study subjects 25(OH) vitamin D levels were retested by Laboratory Corporation of America. The subjects also filled out the same medical symptom questionnaire and the data was compiled. At the beginning of the study, the average baseline 25(OH) vitamin D blood level was 27.02 ng/mL. Current medical guidelines suggest that vitamin D insufficiency begins when blood levels are below 32 ng/mL and optimal disease prevention occurs when blood levels are above 60 ng/mL (REF). Only five study subjects had serum levels above the 32 ng/mL level and two subjects had blood levels less than 11 ng/mL. The majority of subjects had levels in the low to mid 20s (See Table 1). Prior to supplementation 75% of the subjects were deficient in vitamin D and 10% of the subjects were severely deficient (as defined by blood levels below 10 ng/mL).
At the beginning of the study, the average baseline 25(OH) vitamin D blood level was 27.02 ng/mL. Current medical guidelines suggest that vitamin D insufficiency begins when blood levels are below 32 ng/mL and optimal disease prevention occurs when blood levels are above 60 ng/mL (REF). Only five study subjects had serum levels above the 32 ng/mL level and two subjects had blood levels less than 11 ng/mL. The majority of subjects had levels in the low to mid 20s (See Table 1). Prior to supplementation 75% of the subjects were deficient in vitamin D and 10% of the subjects were severely deficient (as defined by blood levels below 10 ng/mL).
 History and Presenting Symptoms
History and Presenting Symptoms
 History and Presenting Symptoms
History and Presenting Symptoms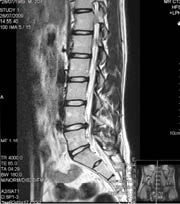
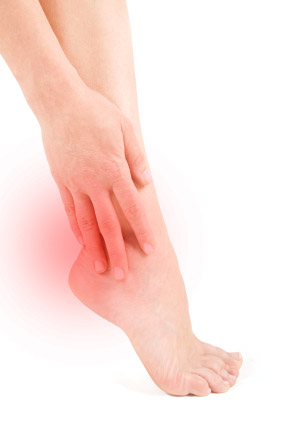
 Based on the examination it was apparent that patient DH had S1 inhibition, which was being expressed by a marked fibularis longus and brevis weakness. Patient DH was compensating for this by distributing more weight on the anterior talofibular ligament and calcaneofibular ligament to check ankle inversion. As such, there was no antagonist control of the stirrup effect created by the tibialis anterior and the fibularis longus. Without this being controlled the tibialis anterior, along with the extensor hallux longus, were overly dorsiflexing the first ray in relationship to the foot upon stance. The excessive lateral wear pattern on the patient’s shoe was associated with a lack of antagonist control of the deep posterior compartment maintaining the foot in an inverted position throughout the gait cycle and stance.
Based on the examination it was apparent that patient DH had S1 inhibition, which was being expressed by a marked fibularis longus and brevis weakness. Patient DH was compensating for this by distributing more weight on the anterior talofibular ligament and calcaneofibular ligament to check ankle inversion. As such, there was no antagonist control of the stirrup effect created by the tibialis anterior and the fibularis longus. Without this being controlled the tibialis anterior, along with the extensor hallux longus, were overly dorsiflexing the first ray in relationship to the foot upon stance. The excessive lateral wear pattern on the patient’s shoe was associated with a lack of antagonist control of the deep posterior compartment maintaining the foot in an inverted position throughout the gait cycle and stance.
 :dropcap_open:I:dropcap_close:got a call from someone who sounded terrible.
:dropcap_open:I:dropcap_close:got a call from someone who sounded terrible.



 awareness of the rate of traumatic brain injuries (TBI) or concussion in today’s youth. This information is mainly directed toward the adult population. Football has always been the sport of primary focus, but recent injuries to NHL star Sydney Crosby has made even more people sit up and take notice. For purposes of this article, our emphasis will be more on the adolescent.
awareness of the rate of traumatic brain injuries (TBI) or concussion in today’s youth. This information is mainly directed toward the adult population. Football has always been the sport of primary focus, but recent injuries to NHL star Sydney Crosby has made even more people sit up and take notice. For purposes of this article, our emphasis will be more on the adolescent.
